When it comes to cardiac care, oxygen therapy has long been an established procedure, particularly for patients experiencing acute myocardial infarction (AMI). However, emerging evidence challenges routine administration, highlighting potential risks, including coronary vasoconstriction and oxidative stress that could worsen outcomes in normoxic patients, or patients who have a normal oxygen level in their blood. This means that titrating oxygen in acute myocardial infarction for nurses demands precision to balance benefits against harms.
This article delves into the pros and cons of oxygen therapy for cardiac patients, helping equip nurses with insights for evidence-based practice.
What is Oxygen Therapy and How Does it Help Patients?
Oxygen therapy involves supplementing patients with additional oxygen when their bodies cannot produce enough oxygen due to illness. Not getting enough oxygen throughout the body can lead to critical issues, such as cerebral hypoxia or brain damage, and even organ damage.
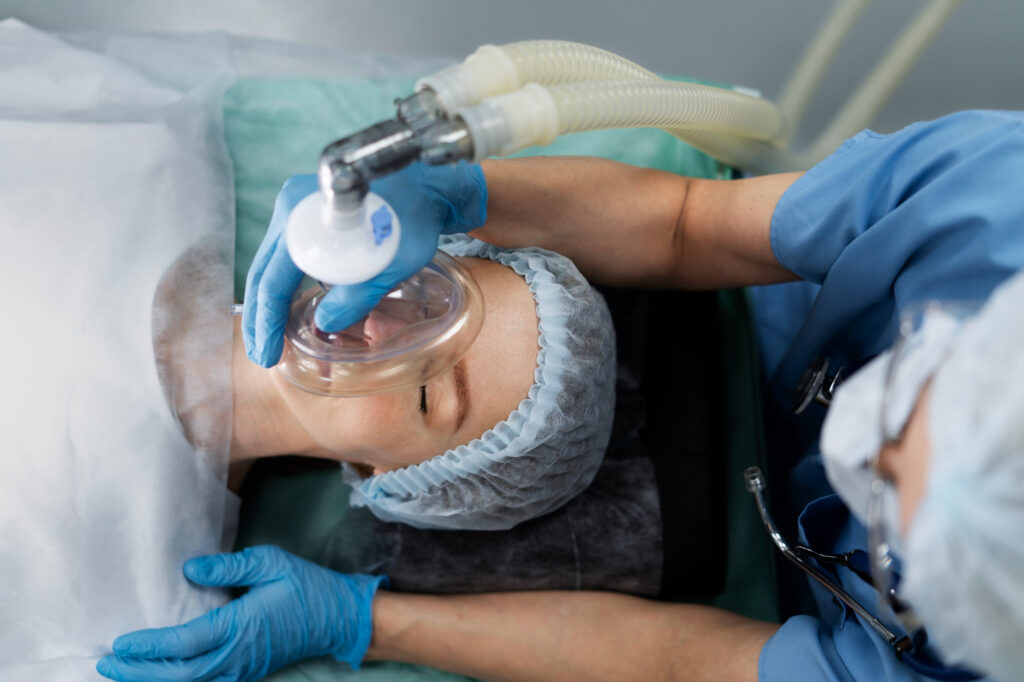
Different kinds of patients benefit from oxygen therapy. Patients with hypoxia or very low oxygen levels suffering from lung conditions such as asthma, pneumonia, sleep apnea, and Covid-19 can be given oxygen therapy to keep their oxygen levels from plummeting. Oxygen therapy is typically given via a mask or a nasal tube from an oxygen tank or machine.
Cardiac patients are also given oxygen therapy when their oxygen levels are really low. When patients have cardiac issues or heart failure, their hearts become weak and are not able to pump blood properly throughout the body. This then leads to the body not getting the right amount of oxygen it needs to function normally. However, it’s important to check the oxygen levels of a cardiac patient before administering oxygen therapy, as too much oxygen can also be harmful to those with heart issues.
When Oxygen Harms: The Physiology of Coronary Vasoconstriction
While low oxygen levels can be harmful, high oxygen levels can also be detrimental to a cardiac patient’s health. This condition is called hyperoxia, or having an excessive supply of oxygen in the blood and tissues, and can lead to oxygen-induced vasoconstriction in the coronary arteries and direct cellular toxicity via reactive oxygen species (ROS). Hyperoxia is not as easily detected or monitored as hypoxia, which can be monitored using a simple pulse oximeter device.
There have been published studies that report on the excessive use of oxygen therapy in cardiac patients. In one study, the researchers posit that the excessive use of supplemental oxygen occurs because medical professionals are not able to properly monitor oxygen tension during oxygen therapy and don’t recognize that oxygen is a vasoactive substance. This means that healthcare professionals, including physicians, don’t recognize oxygen as a substance that can affect the narrowing or widening of the heart’s arteries or blood vessels.
Understanding the Risks of Hyperoxia in Post-Cardiac Arrest
There are also risks of hyperoxia in post-cardiac arrest patients. In a report published in 2018, it is common for cardiac patients who have undergone cardiopulmonary resuscitation (CPR) to experience hyperoxia. This occurs because of a continuous supply of supplemental oxygen even after a successful CPR or the return of spontaneous circulation (ROSC).
In a study published in the AHA/ASA Journals, researchers observed adult patients with cardiac arrest who were mechanically ventilated. They found that 105 out of 280 cardiac patients were exposed to hyperoxia. They observed that a staggering 70% of patients who had hyperoxia experienced poor neurological function at the time of hospital discharge.
Nurses play a crucial role in keeping cardiac patients safe from the harms associated with an overabundance of supplemental oxygen from oxygen therapy. Nurses should closely monitor oxygen saturation levels to avoid both hypoxia and hyperoxia, as well as regularly titrate supplemental oxygen to the lowest effective dose. By staying informed about the risks of excessive oxygen and adhering to updated protocols, nurses are able to make informed clinical decisions and become strong advocates for patient safety in the workplace.